Overview
External cyclopexy ciliary body tear repair is demonstrated in this case of hypotony following Yamane-style intraocular lens fixation. The video shows identification of a ciliary body tear on UBM without an anterior chamber cleft and its surgical repair using a double scleral flap approach. The procedure includes direct visualisation of the tear and suturing of the ciliary body band to the sclera.
Video on YouTube
This video demonstrates external cyclopexy for ciliary body tear repair in a hypotony case following Yamane-style intraocular lens fixation.
If age-restricted, please watch this video directly on YouTube.
Case context
- Prior surgery: Replacement of opacified intraocular lens with Yamane-style fixated intraocular lens
- Scenario: Severe hypotony with UBM-confirmed ciliary body tear and no visible anterior chamber cleft
- Focus of video: External exploration and repair of the ciliary body tear using cyclopexy
Key observations
- External cyclopexy ciliary body tear repair performed using a double scleral flap technique
- Double scleral flap technique enabled direct visualisation of the tear
- Viscoelastic provided intraoperative stability compared to anterior chamber maintainers
- Ciliary body band was sutured to sclera using circumferential bites
- Postoperative course included delayed IOP spike controlled with medication
Transcript
Case Introduction
[00:09] Over the years, I have been referred many patients with hypotony, either from trauma, glaucoma surgery, vitreoretinal surgery, and even chronic uveitis. However, recently I have seen an increasing number of cases associated with secondary sutured intraocular lenses or Yamane-style haptic-fixated intraocular lenses.
The case I am going to present was a particular diagnostic and therapeutic challenge.
Read more
Clinical Presentation And Imaging
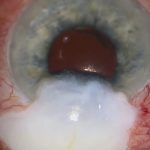
[00:44] This patient developed severe hypotony after an opacified intraocular lens was replaced with a Yamane-style fixated intraocular lens in the right eye.
Five months after surgery, UBM clearly shows a ciliary body tear close to the haptic, though there is no cleft in the angle.
External exploration is required to visualise the extent and location of the tear and its relationship to the haptic, which is essential for accurate closure.
The IOL haptic, but not the tear, is seen with the Ahmed gonio prism. Endoscopy would be required to see the tear.
Surgical Exposure And Flap Creation
[01:33] The conjunctiva is opened in the area of the tear as indicated by the UBM.
The area around the haptic is dissected carefully. The haptic is only covered by conjunctiva, which represents an exposure risk. From the UBM, the scleral course of the haptic is unlikely to be involved in the ciliary body tear.
Nevertheless, the surgeon must be prepared to open the sclera around the haptic if required.
A double scleral flap is fashioned so that the sutures can be buried. I mark approximately 4 mm from the limbus for the posterior margin of the outer flap and then create a partial-thickness scleral flap.
The flap should be longer than the anticipated length of the tear to ensure all of the tear can be visualised and repaired.
I have avoided the scleral exit site of the IOL haptic, as the UBM suggests that the tear does not encompass this area.
The inner flap is then outlined approximately 1 mm inside the outer flap, gently grooving the sclera with repetitive shallow cuts.
Eventually, the groove reaches full scleral thickness so that the suprachoroidal space is entered, as evidenced by the release of suprachoroidal fluid.
The remainder of the flap is opened fully with the blade reversed, cutting upwards to avoid traumatising the choroid or ciliary body.
Intraoperative Stabilisation And Tear Identification
[03:28] A thick cohesive viscoelastic such as Healon GV is generally more useful than an anterior chamber maintainer in this situation.
Anterior chamber maintainers either create a fountain from the tear itself, obscuring the view, or cause uncontrollable choroidal bulging.
Viscoelastic creates a more stable environment in which to close a cleft, or in this case, a ciliary body tear.
The full extent of the tear is now visible under the flap. Having confirmed that all of the tear can be visualised, it can then be closed.
External Cyclopexy Repair Technique
[04:07] This is achieved by suturing the ciliary body band back to the sclera.
This is neither as difficult nor as dangerous as it sounds and is performed by passing the needle through the inner flap and gently engaging the ciliary body band circumferentially.
In this case, I have not engaged the ciliary body band sufficiently with the initial bite, so I will take another before passing the needle back out through the inner flap so that the knot will be located between the inner and outer flaps.
I will usually place three throws on the suture but not lock it down until all required ciliary body sutures have been inserted.
As this is not a long tear, few sutures are required.
The tear appears to be closed adequately, but it is important to check for neighbouring tears.
There is a suspicious area on the other side of the central adhesion. This area is also sutured.
Unlike the previous sutures, I am taking a circumferential bite of ciliary body, which is a more controlled method.
At this point, all of the ciliary body sutures can be locked down.
Flap Closure
[06:40] As this is a relatively small tear, I am fairly confident that it has been closed adequately.
It is important to close the inner flap robustly to prevent dehiscence if there is a postoperative IOP spike.
Here I am using 9-0 nylon. 10-0 is insufficient to prevent wound opening if a very high postoperative IOP spike occurs.
The suture is buried under the inner flap. This is not essential, as the outer flap will cover the sutures.
The inner flap is closed tightly using many closely spaced sutures to maximise postoperative wound integrity.
The viscoelastic is then removed.
The outer flap and conjunctiva are glued back in place using fibrin tissue glue. One or two sutures may also be placed in the conjunctiva if required.
Postoperative Course And Outcome
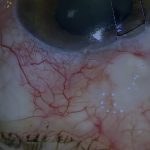
[07:54] This is the appearance three weeks after surgery. The pressure remained low for the first 13 days but then increased to over 40 mmHg, which was rapidly controlled with medication.
This is the appearance three weeks after surgery and eight days after the pressure spike.
There is a clear difference on UBM between the preoperative and postoperative appearances.
Key Learning Points
[08:40] This case was unusual in that there was no visible cleft in the anterior chamber and no visible cause of the hypotony.
The ciliary body tear was clearly visualised with UBM, which proved to be of great diagnostic value.
The tear was successfully repaired, restoring intraocular pressure and improving the patient’s vision.
There has been an increasing number of cases associated with this type of lens fixation in recent years. This may be a less recognised complication that clinicians should be aware of, and importantly, it can be repaired.
For outcome benchmarking, see the International Glaucoma Surgery Registry.