Overview
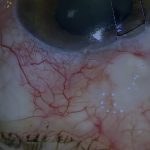
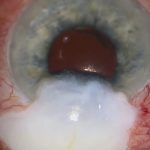
External cyclopexy ciliary body tear repair is demonstrated for chronic hypotony following a Yamane scleral fixated IOL procedure. This case describes persistent hypotony after prior retinal surgery and scleral fixated IOL insertion. UBM suggested a retroiridial ciliary body defect, which was confirmed intraoperatively. Surgical repair using external cyclopexy and secure flap closure resolved the hypotony.
Video on YouTube
This video demonstrates diagnosis and surgical management of a ciliary body tear causing chronic hypotony after Yamane IOL surgery.
If age-restricted, please watch this video directly on YouTube.
Case Context
- Prior surgery: Multiple retinal procedures, intraocular lens exchange, and Yamane scleral fixated IOL insertion
- Scenario: Persistent hypotony with tilted IOL and inconclusive gonioscopy, with UBM suggesting a retroiridial ciliary body tear
- Focus of video: Identification and repair of a ciliary body tear using external cyclopexy technique
Key Observations
- Increasing referrals of ciliary body tears and cyclodialysis clefts associated with scleral fixated IOL techniques [00:17]
- UBM suggested a retroiridial ciliary body tear from 2 to 6 o’clock, not confirmed on endoscopy [00:48]
- Intraoperative exploration revealed the tear between 2 and 4 o’clock despite misleading imaging [03:00]
- The defect appeared round and possibly related to a previous vitrectomy port rather than direct trauma
- Secure suturing of the ciliary body to sclera reduced suprachoroidal drainage and resolved hypotony
Transcript
Case Introduction and Context
[00:17] Recently, I have been referred increasing numbers of ciliary body tears and cyclodialysis clefts related to either Yamane or other scleral fixated intraocular lens techniques. The case I am about to present is the second Yamane-related retropupillary ciliary body tear that I have seen in six months.
These cases are particularly interesting to fix, as you will see, and I do hope you find this one interesting.
Read Full Transcript
Clinical Presentation and Imaging Findings
[00:48] In this video, I am going to describe another case of chronic hypotony after a Yamane-type scleral fixated intraocular lens and how the cause of the hypotony was diagnosed and how it was managed. This eye developed persistent hypotony after a Yamane-style scleral fixated IOL insertion.
There was a prior history of multiple retinal procedures, intraocular lens exchange, and choroidal decompensation. In addition, the IOL was tilted.
Gonioscopy failed to reveal a cyclodialysis cleft. UBM suggested a retroiridial ciliary body tear from 2 to 6 o’clock, but less obvious than the similar case that I recently posted.
Endoscopic Assessment and Surgical Exploration
[01:41] I therefore decided to have a look with the endoscope. Pars plana, pars plicata, and Yamane IOL haptic all seemed to be in order. Despite an extensive search as close to the back of the iris as possible, I could find no tear.
The only remaining option was therefore to raise a flap in the area that was suspicious on UBM. A partial thickness scleral flap is raised 4 mm from the limbus, encompassing all four clock hours marked as suspicious on UBM.
A deep flap is then cut half to 1 mm inside the confines of the superficial flap. The suprachoroidal space is entered gently with the blade upward to avoid traumatising the choroid or ciliary body.
Although the superficial flap had been opened from 2 to 6 o’clock as suggested by UBM, I have only opened the deep flap from 3 to 6 o’clock to try and avoid disturbing the Yamane IOL haptic.
Identification of the Ciliary Body Defect
[03:00] Unfortunately, the UBM seems to have been misleading and the ciliary body tear is actually between 2 and 4 o’clock. As a result, I will need to extend the deep flap much closer to 2 o’clock.
This is of course more difficult when the eye is soft, though extending a partial thickness scleral flap is much easier than extending a full thickness flap.
As mentioned in previous videos, I tend to use cohesive viscoelastic rather than an AC maintainer. An AC maintainer may result in a fountain through the tear and also dramatic choroidal bulging obstructing closure. I find that viscoelastic tends to give greater stability. I usually use Healon GV Pro or Healon 5 Pro.
With the flap fully open, the full extent of the tear is visible. However, with its round appearance, this does not really look like a traumatic tear. The portion of ciliary body traversed by the Yamane IOL haptic also looks altered, but this is likely due to the surgery.
Aetiology and Surgical Repair Technique
[04:11] I therefore need to open up more to expose this area fully, which necessitates extending both flaps. When fully exposed, any surgical trauma to the choroid or ciliary body appears to be minor and located away from the ciliary body hole.
Given that the hole is round, I wonder if it might be from a previous vitrectomy port. Although the position is very anterior, I have seen a small number of cases of chronic unexplained post-vitrectomy hypotony over the years. I have seen one case where the pars plana portion of a vitrectomy port was draining into the suprachoroidal space, and this seems to be the likely aetiology here, probably precipitated by the recent scleral IOL fixation procedure.
Irrespective of the cause, this hole needs to be closed. This is achieved by suturing ciliary body band back to sclera.
It is important to use a robust suture. I currently use 9-0 nylon. 8-0 is also acceptable but a little more coarse. I have seen two cases of wound failure after high IOP spikes when 10-0 nylon was used with clefts, so I avoid 10-0.
The ciliary body defect must be secured tightly to sclera to prevent further suprachoroidal drainage.
Closure Technique and Intraoperative Assessment
[06:19] I will often test the closure with Vision Blue in the anterior chamber. Ideally, the closure should not be completely watertight because viscoelastic has been used and there is a chance of a high IOP spike.
But on the other hand, there should be no gape. As there is still quite brisk drainage, more sutures are required. Now there is only slow seepage of aqueous from the tear, which is better.
So it is time to close the deep flap. The deep flap must be closed tightly with robust sutures. This is to ensure there is no risk of wound dehiscence should the pressure spike dramatically after surgery.
As previously mentioned, I use 9-0 nylon to close the tear, but it is also important to use a robust suture to close the flap. 10-0 nylon is insufficient should a high postoperative IOP spike occur, so ideally 9-0 or even 8-0 nylon should be used.
The deep flap is sutured very tightly with many sutures to eliminate any risk of dehiscence if the IOP elevates later.
Eventually the deep flap is secure, and the superficial flap is closed with fibrin glue to cover the deep flap and ciliary body suture knots. The conjunctiva is then closed with fibrin glue.
Postoperative Outcome and Clinical Implications
[09:37] One month after surgery, the IOP is 14 mmHg without glaucoma medication. The visual acuity is still limited at count fingers because of the corneal oedema and tilted intraocular lens, both of which will need to be addressed in the long term.
But the chronic hypotony problem has now been removed from the equation. Unfortunately, the patient has not suffered from a postoperative intraocular pressure spike.
In the last three years, I have been referred five cases of cyclodialysis clefts and ciliary body tears related to either Yamane or other scleral fixated intraocular lens techniques. I do not know if this has just been bad luck, increasing use of these techniques, inexperience with the techniques, or if it is an innate risk with these techniques.
No matter what the cause, I think it is important to know how these can be diagnosed and especially important to know that they can be repaired and the hypotony fixed.
For outcome benchmarking, see the International Glaucoma Surgery Registry.