Overview
PRESERFLO revision bleb failure technique demonstrates surgical revision of a scarred MicroShunt with restoration or conversion to tube implantation. This video shows revision of a failed PRESERFLO MicroShunt due to scarring or bleb failure. It includes examples of limited fibrosis and dense capsular scarring with differing surgical approaches. Techniques for flow modulation and device removal during glaucoma drainage implant surgery are also demonstrated.
Video On YouTube
Step-by-step surgical techniques for revising and removing a PRESERFLO MicroShunt in cases of bleb failure.
If age-restricted, please watch this video directly on YouTube.
Case Context
- Prior surgery: PRESERFLO MicroShunt implantation
- Scenario: Failure to control IOP due to scarring or bleb failure
- Focus of video: Revision techniques, flow control, and removal during glaucoma drainage implant surgery
Key Observations
- [00:42] Minimal fibrosis with absent bleb suggests lack of aqueous contact with subconjunctival space
- [02:46] Removal of fibrous tissue restores free drainage through the PRESERFLO
- [03:24] Dense Tenon’s capsule formation is a common finding in failed cases
- Partial occlusion with polypropylene ripcord used to reduce excessive aqueous flow
- Removal of PRESERFLO with tunnel closure using fascia lata or suturing during tube implantation
Transcript
Overview And Indication
[00:00] Today I'm recording from the World Glaucoma Congress in Honolulu where we've been discussing minimally invasive bleb surgery. Anyone who performs minimally invasive bleb surgery on a regular basis, such as a XEN or PRESERFLO MicroShunt, will occasionally have to revise the procedure due to scarring or bleb failure.
In this video, I'm going to describe briefly how I revise a PRESERFLO MicroShunt should it have failed from scarring. In this video, I'm going to describe how I revise a PRESERFLO MicroShunt that has failed to control the intraocular pressure.
Read Full Transcript
Initial Revision Approach And Intraoperative Findings
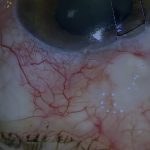
[00:42] When revising a failed PRESERFLO, I will usually start at the limbus and try and separate the conjunctiva from the bleb. Here, the PRESERFLO can be seen intact. Surprisingly, there seems to be little scarring in this case and no bleb. It appears almost as if aqueous was never in contact with a subconjunctival space.
The overlying tissue is even quite mobile, which is particularly unusual for a revision. I reapply mitomycin C (MMC) for 3 minutes. The sponges are spaced out quite widely and posteriorly where possible. The intact Tenon’s or PRESERFLO capsule prevents MMC from accessing the anterior chamber. In this case, there's still some subconjunctival bleeding which is not ideal.
Contact with blood or serum protects fibroblasts from the cytotoxicity of MMC, reducing its effect. The MMC is irrigated away with 20 mL of BSS. At this point, the tissue overlying the PRESERFLO can be incised, taking care not to damage the device.
On first inspection, there seems to be less fibrosis around the device than one might expect in this situation. Nevertheless, it is embedded in some fibrous tissue that must be carefully dissected off the device, after which the PRESERFLO starts to drain normally. Here a very typical stocking of fibrous tissue is removed from around the PRESERFLO, and now it can be seen to be draining freely.
Dense Capsule Revision And Flow Modulation
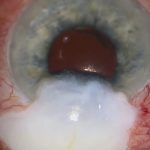
[03:24] Here's another case. The conjunctiva is opened in a similar manner. In this case, the PRESERFLO is barely visible through a dense overlying capsule. This is a more typical finding than the lighter fibrosis in the previous case.
This dense capsule is not an uncommon finding after exposure of Tenon’s capsule to aqueous humour and is also seen during trabeculectomy revision. The thick capsule is dissected away from the PRESERFLO after the application of MMC and irrigation with BSS.
In this case, I was concerned that the rate of aqueous drainage was excessive for this elderly patient. I therefore decided to partially occlude the PRESERFLO with a 3-0 polypropylene ripcord. First, a scleral bite is made just behind the posterior opening of the PRESERFLO. Then the loop is buried in a peripheral corneal groove to facilitate removal later.
The needle is then cut off cleanly to avoid a bulb at the end of the suture and the suture inserted into the PRESERFLO. The length of the suture that is inserted will depend on how much flow restriction results. Once it has been confirmed that there's still adequate residual drainage, the suture loop is shortened.
This often has the added benefit of drawing the PRESERFLO down towards sclera so it sits less proud. The conjunctiva is closed in one layer as there's no distinct Tenon’s, having become integrated into the bleb capsule. If there is a separate Tenon’s layer, it probably should be advanced and sutured separately, but not to the limbus.
Revision carries a risk of ptosis and diplopia. Excessive conjunctival and Tenon’s advancement are important risk factors for this. The conjunctiva can then be closed separately.
Removal And Tube Implantation Strategy
[06:49] Occasionally I have to remove one completely and put in a glaucoma drainage implant. In the next part of the video I’ll show briefly my techniques for performing that procedure, focusing on how I manage the pre-existing PRESERFLO at the same time as the glaucoma implant.
If one PRESERFLO fails to control the pressure, a second is unlikely to work better than the first, especially in a high scarring ethnicity such as this Afro-Caribbean patient. I would usually also remove the PRESERFLO at the same time as inserting the glaucoma implant in order to protect the endothelium from the risk of attrition by the presence of extra implants.
My standard approach to implanting a glaucoma drainage device in the case of a failed PRESERFLO is to avoid opening the capsule over the PRESERFLO until I've completed the implantation and checked the aqueous flow of the implant. In this case, I'm now opening the capsule over the PRESERFLO. Until now, this has been completely encapsulated, which protects the eye from hypotony at the time of implantation.
After removing the PRESERFLO, one can see that the tunnel is quite thin-walled and now it is draining quite profusely. There are two ways to close an overdraining tunnel. I find bunging it with a piece of fascia lata, pericardium, or donor sclera to be more effective in many cases than suturing, especially if the tunnel is thin.
This is quite a physical process where one takes a tapered piece of fascia and pushes it very tightly into the tunnel. After reinflating the anterior chamber, the entry site is now watertight. The fascia bung is secured with fibrin glue, which is a very handy way to keep it in place. After checking the entry site with fluorescein, it is no longer leaking, but the implant is still draining adequately and at roughly the right rate.
Alternative Techniques And Combined Device Strategy
[09:56] In this case, the PRESERFLO is already exposed and draining, but because of its innate resistance it hasn’t caused very dramatic hypotony. I was able to implant the glaucoma device in the usual fashion. The tube is secured to the sclera with 9-0 nylon.
At this point the PRESERFLO is removed easily. In this case the tunnel is more robust than in the previous case, not leaking significantly and easier to close with 10-0 nylon. Hydrating the tunnel also helps seal it. Once the tunnel is closed, I proceed with the conclusion of the implantation. I bury the 6-0 Prolene ripcord in a peripheral corneal loop to facilitate later removal.
I cover the tube and the previous PRESERFLO entry site with donor fascia lata, securing it with fibrin tissue glue, and then close the Tenon’s and conjunctiva with a combination of glue and sutures.
An alternative technique in cases where there has been a failed PRESERFLO is to connect a Baerveldt tube to the PRESERFLO, which is not unreasonable. I don’t tend to do this because the PRESERFLO has a few mmHg of innate resistance which will be added to any capsular resistance.
In theory, adding a Baerveldt to a PRESERFLO will result in slightly higher pressures in the long term. However, to illustrate the technique, I’m showing a case where a Baerveldt implant was removed because of hypotony in a young uveitic patient and later reinserted attached to a PRESERFLO.
In this case, the additional resistance of the PRESERFLO is used to prevent chronic hypotony. The Baerveldt is trimmed so that there is a millimetre or two overlap between the end of the tube and the PRESERFLO. A 3-0 monofilament nylon ripcord remains within the Baerveldt.
The junction of the Baerveldt and PRESERFLO is secured to sclera with nylon. The junction is covered with a donor fascia lata patch graft secured with fibrin glue, and the conjunctiva is closed with a combination of glue and 10-0 nylon sutures.
These are the techniques for revising a PRESERFLO and managing its removal when implanting a glaucoma drainage device.
For outcome benchmarking, see the International Glaucoma Surgery Registry.