Overview
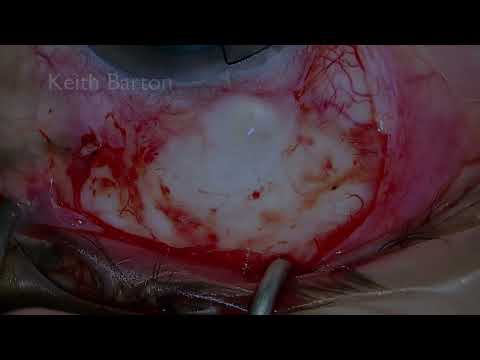
Trabeculectomy revision hypotony maculopathy is managed here with bleb excision, scleral flap repair, and pericardial patch grafting. The case demonstrates excision of an avascular bleb area and identification of a scleral flap perforation. A pericardial patch is used to restore integrity and allow controlled aqueous outflow. Adjustable suturing techniques are used to balance flow and achieve watertight closure.
Video On YouTube
Step-by-step surgical revision of trabeculectomy for hypotony maculopathy using a pericardial patch and controlled flow techniques.
If age-restricted, please watch this video directly on YouTube.
Case Context
- Prior surgery: Trabeculectomy with MMC
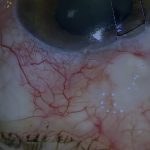
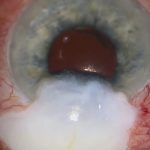
- Scenario: Hypotony maculopathy presenting more than eight years after surgery with a large diffuse posterior bleb
- Focus of video: Revision of bleb and scleral flap perforation using pericardial patch and adjustable suturing
Key Observations
- Anterior avascular bleb area is excised before addressing the larger posterior bleb
- Bleb cavity extends significantly posteriorly explaining severity of hypotony [00:23]
- Clear perforation identified in anterior scleral flap requiring patch repair [01:25]
- Pericardial patch width and edge suturing control anterior and posterior aqueous flow
- Conjunctiva closed tightly at limbus with running sutures to ensure watertight seal [04:26]
Transcript
[00:00] In this video I describe a trabeculectomy revision for hypotony maculopathy. A patient in their 50s presented with hypotony maculopathy more than eight years after trabeculectomy with MMC.
Although there is a very large diffuse posterior bleb, this anterior focal avascular area should first be excised.
Read Full Transcript
Revising a Trabeculectomy for Hypotony with Pericardium
Case Presentation and Hypotony Maculopathy
Bleb Dissection and Capsule Excision
[00:23]
After delineating the avascular area, the conjunctiva is separated posteriorly from the remainder of the bleb, which is quite extensive. After achieving adequate haemostasis, the bleb capsule is excised in the avascular area.
Underneath there is another layer of capsule, which is frequently the case. Bleb cavities are often not just simple cysts. This is also excised. Note how the bleb cavity extends much further back than the excised area. The size of this cavity explains the degree of hypotony.
Identification of Scleral Flap Perforation
[01:25]
After tidying the area, further haemostasis is achieved and the anterior chamber is inflated so the flap can then be inspected properly.
There is a clear perforation in the anterior portion of the scleral flap. This is not something that can be easily sutured. It must be patched, and in this case human donor pericardium is used.
Pericardial Patch Placement and Flow Control
[01:55]
The anterior edge must be sutured until watertight, or aqueous will be directed to the limbal conjunctival margin. After checking that the front edge is watertight, the back is closed such that it can be adjusted to allow some flow.
The posterior bleb capsule, Tenon’s and conjunctiva are mobilised so the patch can be secured and to facilitate conjunctival closure. The patch, as in this case, must be wide enough to prevent lateral flow, with sutures at the edges reducing posterior flow.
Tightening the back has now made the front edge leak again, so both need to be addressed. A releasable 10-0 nylon suture in the posterior edge offers some potential to adjust postoperative aqueous drainage.
Suture Adjustment and Tension Balancing
[03:00]
After an initial loop is buried in a peripheral corneal slit, the releasable knot is tied with four throws, leaving the loop short. Both are adjusted to get the right tension, eliminating flow unless the posterior edge of the patch is gently depressed.
The new tension on the posterior edge has caused the anterior edge to drain spontaneously again. The front edge is tightly secured with multiple 10-0 nylon mattress sutures to eliminate flow even under tension.
Final Drainage Control and Conjunctival Closure
[04:26]
As a result, there is now significant spontaneous drainage from the back of the patch, which requires further attention. Two additional interrupted sutures are added to the back of the patch to reduce, but not eliminate, drainage completely.
The conjunctiva and Tenon’s are mobilised extensively to ensure a tension-free closure, avoiding ptosis or even diplopia. As there is a higher risk of limbal leakage when a patch graft is used, the conjunctiva must be closed tightly at the limbus.
First, the conjunctiva is stretched laterally using 10-0 nylon wing sutures. The wing suture is extended into a locked running suture to close the lateral gap produced by the limbal conjunctival margin.
The limbal conjunctival margin is then closed with a 10-0 nylon locked running suture to ensure a watertight limbal seal.
For outcome benchmarking, see the International Glaucoma Surgery Registry.