Overview
This surgical video demonstrates how a Paul Glaucoma Implant can be successfully positioned in an eye with a pre-existing 360° scleral buckle. Professor Keith Barton details the safe removal of a long-standing buckle, preparation of the scleral bed, mitomycin-C application, and secure tube insertion with patch graft reinforcement. The case highlights key considerations for space management, scleral integrity assessment, and conjunctival repair in complex secondary glaucoma surgery.
Video on YouTube
Paul Glaucoma Implant placement after scleral buckle removal in a scarred eye, showing space creation, MMC use, secure tube, and conjunctival repair.
If age-restricted, please watch this video directly on YouTube.
Key points
- Assess the extent of any existing scleral buckle before selecting a quadrant for implant placement.
- Buckle removal can create adequate orbital space but requires confirmation of healthy underlying sclera.
- Apply mitomycin-C judiciously and irrigate thoroughly to reduce post-operative scarring risk.
- Secure the Paul Glaucoma Implant tightly to minimise plate movement and potential encapsulation.
- Use fascia lata patch grafts and fibrin glue to reinforce areas of conjunctival thinning and prevent tube erosion.
Transcript
Paul Glaucoma Implant: Scleral Buckle Removal and Placement
Occasionally there is simply no space for a glaucoma drainage device because of previous retinal surgery. The case I am going to show is one such example, and I will describe how I managed what initially seemed to be an almost impossible situation. I hope you find it useful. [00:31]
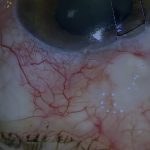
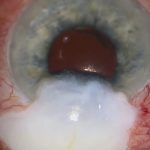
This eye, with a history of retinal detachment surgery, required a tube implant for secondary open-angle glaucoma. The conjunctiva was very scarred, and there was a scleral buckle of unknown nature and extent. The buckle had been implanted twenty-four years earlier at another hospital and appeared to extend 360°. The retina subsequently reattached, requiring silicone oil that was later removed. The patient also had piggyback lenses, and intraocular pressure (IOP) became uncontrolled about five years ago. This was treated with micropulse laser trabeculoplasty, but the IOP was only partially controlled on acetazolamide.
Read more
This video demonstrates management of a complex glaucoma case where a pre-existing scleral buckle obstructed tube placement. Professor Keith Barton shows the safe removal of a 24-year-old buckle, preparation of scleral space, mitomycin-C application, Paul Glaucoma Implant placement, and conjunctival repair using fascia lata grafts. Key insights include assessing scleral integrity before buckle removal and reinforcing exposed areas to prevent tube erosion.
Assessing the Buckle and Deciding on Removal
Each quadrant was examined for conjunctival mobility and available orbital space to accommodate a Paul Glaucoma Implant (PGI). There was no conjunctival mobility and no space for a PGI in any quadrant because the buckle appeared bulky. As the buckle had been in place for twenty-four years and the retina was stable, it was contributing nothing to retinal protection. It could therefore be safely removed, provided the underlying sclera was intact. Despite the obstacles, the superotemporal quadrant seemed the best option for implant placement, but this would be impossible without buckle removal. I decided to open the conjunctiva and inspect the sclera beneath the buckle. [03:00]
Exposure and Dissection
A wide limbal peritomy was performed, and the conjunctiva and Tenon’s capsule were dissected back to the capsule around the buckle. Fortunately, the sclera beneath appeared normal and healthy. The buckle was then dissected free. Interestingly, some buckle sutures were still present after twenty-four years. There was no encircling band holding the buckle in place, which soon became clear when the buckle was cut and withdrawn. This type of buckle was historically used for indentation over a tear in one quadrant, but in this case it had been placed through 360°, explaining the lack of space in the orbit.
Creating Space for the Paul Glaucoma Implant
The anteroposterior depth of the PGI plate is greater than the width of the removed buckle. Therefore, the posterior capsule of the buckle had to be incised to accommodate the PGI plate. Scleral buckle capsules tend to be very dense and difficult to incise, often requiring forceful sharp dissection in areas not easily visualised. A thin linear area of scleral thinning was visible secondary to buckle indentation, but this was not extensive enough to be a major hazard. I applied relatively high-dose mitomycin-C (MMC) as with most tube procedures, except in eyes at high risk of hypotony. Two sponges were used, soaked in a total of 0.8 mL of 0.5 mg/mL MMC. Because this was placed far from the limbus, it did not cause conjunctival avascularity or increase the risk of erosion. The MMC was then irrigated with 20 mL of balanced salt solution. [05:25]
Implant Placement and Tube Insertion
The PGI plate was inserted beneath the adjacent superior and lateral rectus muscles. There appeared to be ample space for the plate, which moved freely without restriction. The plate sat approximately 10 mm from the limbus—an ideal position—and was secured tightly to the sclera with two 9-0 Prolene sutures to prevent movement and reduce the risk of encapsulation. The tube was trimmed to length, and the anterior chamber was entered with a 25-gauge needle as close as possible to the iris plane. The tube was inserted into the anterior chamber and fixed to the sclera with 9-0 nylon mattress sutures. I prefer to bury the knots in the sclera, or at least keep them away from the tube, as knots overlying the tube are a common cause of tube erosion. [07:00]
Patch Grafting and Closure
A human donor fascia lata patch graft was secured over the tube and ripcord with fibrin glue. Another piece of fascia lata was positioned in the fornix to protect the plate beneath a large overlying conjunctival defect. The graft was pulled forward, positioned correctly under the defect, and fixed in place with fibrin glue. The conjunctiva, also glued, was carefully sutured closed with locked continuous 10-0 nylon sutures, ensuring that the plate and tube were protected from the area of the conjunctival buttonhole. [08:20]
Summary and Key Learning Points
Removing a large buckle can create substantial space for glaucoma drainage device implantation. The main risk of buckle removal is not retinal redetachment—assuming the buckle has been in place for many months or years—but that the sclera beneath might be very thin and prone to perforation. This must be assessed first. Additionally, a large conjunctival buttonhole can be repaired with an underlying patch graft to prevent tube erosion in that area. [09:00]
For outcome benchmarking, see the International Glaucoma Surgery Registry.